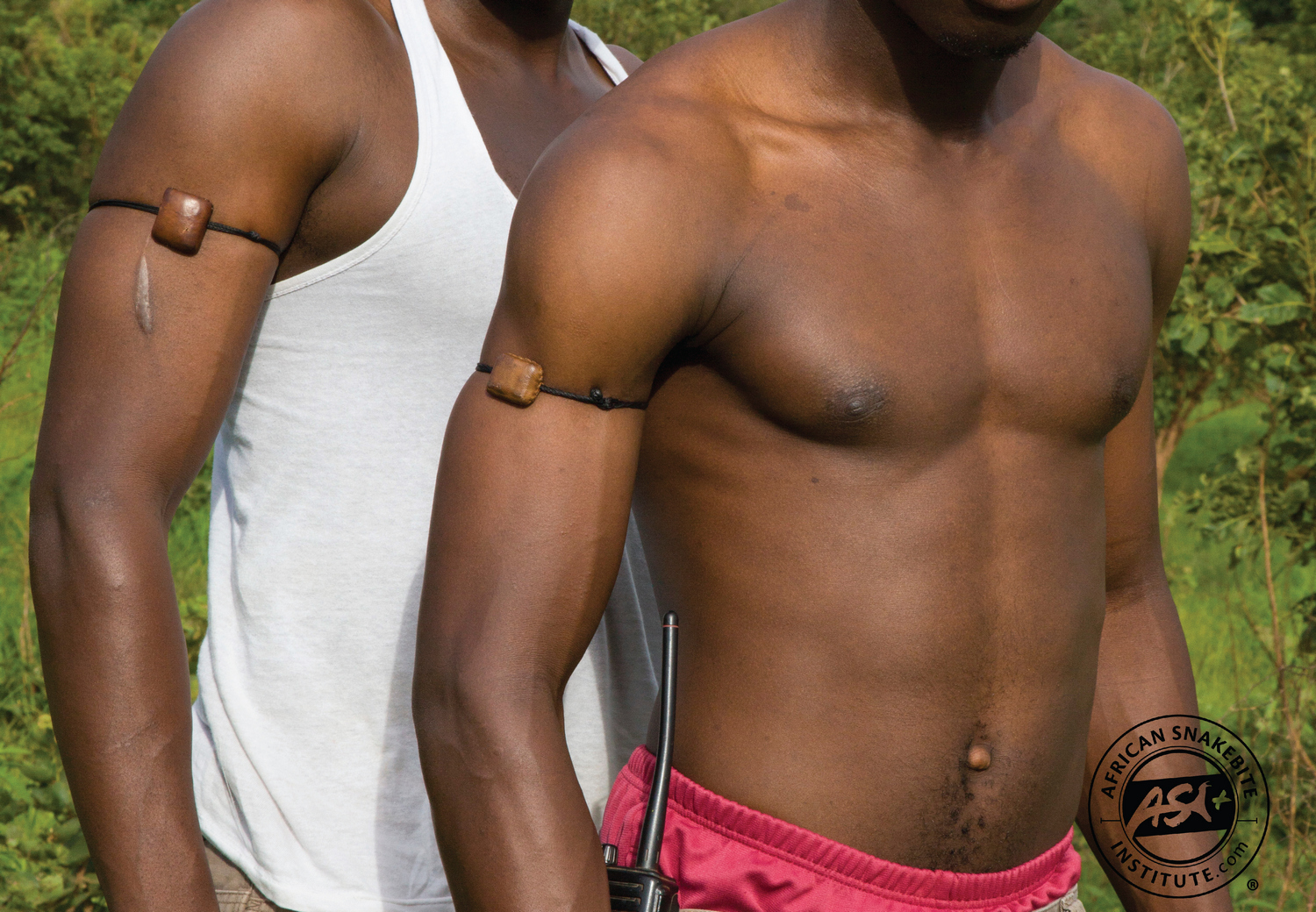A recent social media post claimed that, following a snakebite, chewing the bark of a cashew nut tree would neutralize the venom of the snake and ensure the full recovery of the victim. In many tropical African countries, cashew nut trees are common and often line the streets around villages. It would be an ideal first aid for snakebite, if true. Unfortunately, there is no evidence that it works and furthermore, raw cashew nuts and the bark contain urushiol, a toxin known to cause allergic reactions in humans.
The World Health Organization estimates that deaths by snakebite in sub-Saharan Africa range between 20 000 – 32 000 each year. This is based on available data and is quite likely an underestimation. Not all snakebite victims are treated in hospitals, especially so in poorer countries and rural areas. Many are treated with traditional remedies and die before ever reaching a hospital. These deaths are not always documented or reported.
Snakebite in Mozambique are estimated to cause around 300 deaths per year. A recent publication conducted just over a thousand household surveys in the Cabo Delgado province in northern Mozambique and estimated that there are over 6000 bites per year, and around 800 deaths, just in that province. They extrapolated this data and conservatively suggested that there are around 69 000 bites and almost 9 000 deaths a year – just in Mozambique!
Most of the population in Mozambique (around 68%) live in rural areas and rely on subsistence farming. These people are often exposed to snakes, and many are bitten. Unfortunately, around 60% of bites are treated by traditional remedies. Only 15% seek medical attention at hospitals. Around 25% die before reaching hospitals.
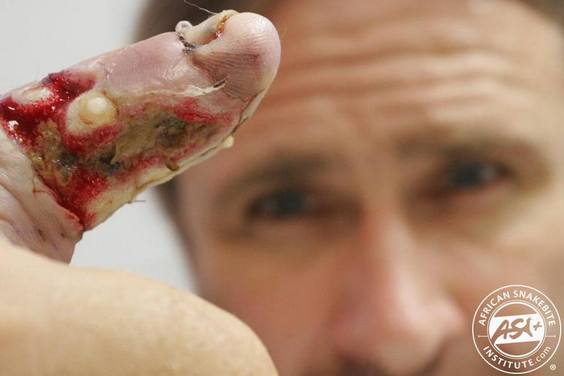
In the Benue Valley of northern Nigeria, snakebite is the leading cause of morbidity and mortality among farmers and hunters (Warrell, 2008). Morbidity from snakebite often leads to the loss of limbs and will negatively affect a farmer’s ability to provide for his family.
Treating snakebite in a hospital, even without the use of antivenom, is quite manageable and for most bites (cytotoxic – such as Puff Adders and Mozambique Spitting Cobras), requires careful monitoring of fluids, managing swelling and tissue damage as well as organ failure. For neurotoxic bites (like Black Mambas) it requires careful management of breathing. A paper from Ngwelezane Hospital in rural KwaZulu-Natal had 879 snake bites over five years and not a single fatality. Another paper from rural KZN had 164 patients with no deaths (Coetzer & Tilbury, 1982) and Sloan et al. (2007) interviewed 50 snakebite patients in hospitals and none died. Snakebite in hospital is treatable and mostly with a good outcome.